
| :: Home :: | |
| :: Contact :: | |
| :: Current issue :: | |
| :: Past issues :: | |
| :: For authors :: | |
| :: Links :: | |
| :: Search :: | |
|
Editor: |
|
Vol. 9 No. 3 |
December 2007 |
Commentary
Implementation of a nurse-driven topical analgesic protocol: Two steps forward, one step back
Tracy Ann Pasek, Dawn Thomas, Indira Khimji, Carol Schmitt, Ann Spence and Rebecca Hanni
Nurses are best prepared to be the focal point for pain assessment and clinical decision-making regarding the use of topical analgesics for painful procedures. Pain during hospitalization is pervasive and nurses are the logical common points of integration among care providers for optimal pain management. A nurse-driven analgesic protocol for children undergoing venipuncture and intravenous cannulation offers measurable benefits to the quality of care for what remains an under-treated population.
Once a child enters the hospital, whether it occurs through an ambulatory, emergency, acute or critical care setting, procedural pain is virtually inescapable. Venipuncture and intravenous cannulation procedures are needed with most medical, surgical and trauma conditions. In fact, it is common for a child with a complex disease process to experience these painful procedures more than once during the same hospitalization.
Care providers perceive the duration of a topical analgesics onset of action as an impediment to the timely flow of patients through a busy, fast-paced emergency department. Intravenous cannulation is considered merely a daily event in the life of a hospitalized child while acute care nurses may identify procedures as those requiring frequent vital sign monitoring and American Society of Anesthesiology (ASA) class assessment (e.g. bone marrow aspiration, interventional radiologic procedures). Intensive care units steadily function in a stat mode, so even when venipuncture can be anticipated, pre-emptive analgesia is often bypassed.
Taddio and colleagues (2005) emphasize the short-term consequences of untreated pain for diagnostic and therapeutic procedures. These include pain during the procedure, lack of cooperation by the child, unsuccessful procedure attempts, repeated attempts, additional pain and a prolonged total procedure time (Taddio et al., 2005). Conditioned anxiety responses and increased pain perception are two of several long-term negative outcomes from untreated procedural pain (Taddio et al., 2002).
The nursing profession is committed to the provision of comfort and the prevention of suffering, a key component being the administration of analgesic medications (American Nurses Association, 2001). Every effort should be made to alleviate or mitigate childrens pain, especially that of procedures, and clinicians have an ethical responsibility to provide full pain treatment; failure to do so amounts to substandard and unethical practice (Pitetti, 2005).
The implementation of pain management protocols has been suggested as a measure to change pain culture and maintain the treatment of pain as a high priority (Kennedy & Luhmann, 1999; Meunier-Sham & Ryan, 2003). In general, protocols should ensure patient care does not fall below an established standard of care. Providing they are not too restrictive and foster clinical decision-making, nursing protocols promote individualized patient care and advance nurse autonomy (Flynn, 2005). Zempsky and colleagues (2004) recommend anticipatory models for procedural pain and topical analgesic protocol adaptation. An international group of pain experts note that individualized analgesic protocols may arise from evidence-based guidelines for the prevention and management of newborn pain (Anand, 2001).
While the literature is replete with recommendations for the implementation of pain protocols, a gap remains between what are known to be effective, easily implemented pain management strategies and what is actually practiced (MacLean et al., 2007). Nurses must recognize the value of nursing protocols and how they can close the knowledge-practice gap, thereby achieving improved pain management. The following description of a quality assurance project offers a detailed example of such an initiative.
Background
The authors sought to evaluate the effectiveness of a nurse-driven protocol to increase topical analgesic use for children experiencing venipuncture and intravenous cannulation. The goals of this project included: (1) to standardize pain management for venipuncture and intravenous cannulation procedures by means of a nurse-driven topical analgesic protocol; (2) to eliminate barriers associated with preemptive analgesia for venipuncture and intravenous cannulation; and (3) to facilitate clinical nurse autonomy related to pain management for venipuncture and intravenous cannulation procedures.
At the inception of the project, a nurse intravenous (IV) team had been functioning for one year at this university-affiliated hospital. The team primarily services acute care patients with infrequent consults from the emergency department and three intensive care units (neonatal, pediatric, and cardiac units). The team is staffed 20 hours a day excluding the hours between 0130 and 0530. Currently, their services total approximately 950 per month; greater than 90% of these include venipuncture and intravenous cannulation. These two procedures were chosen as a starting point because of their similar nociceptive properties and because of their high volume relative to other IV team services.
The organization did not have a pain standard of care for venipuncture or intravenous cannulation. In 2005, before the project started, the nurse IV teams rich database revealed that they used a topical analgesic for only 1.9 to 3.4% of children. In 2006 usage averaged 4%. (These data do not capture topical analgesic use by non-IV team nurses who perform these procedures.)
The protocol (Table 1) requires L.M.X.4® (lidocaine 4% topical anesthetic cream, Ferndale Laboratories). This formulation was added to the hospital formulary in 2003 at the recommendation of an anesthesiologist for the following advantages over the existing related compounds (lidocaine injection and EMLA®): (1) fewer severe adverse effects than existing agents; (2) shorter onset of action; (3) increased effectiveness; (4) indications for use in children < 12 years; and (5) lower cost. EMLA® was retained during a transition period for children and families who may have been accustomed to its use.
Table 1. Summary of the L.M.X.4® Pain Management Nursing Protocol* for Venipuncture and Intravenous Cannulation
Patient Eligibility: |
||
|
|
|
|
|
|
|
|
|
Protocol Steps: |
||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Protocol approval
The Pain Innovation Team (PIT) approved the protocol. This multidisciplinary group comprises professional staff nurses or Pain Resource Nursesa designation connoting more responsibility than traditional committee representatives common to hospital groups. Physicians, pharmacists, child life specialists, nurse educators and a nurse practitioner also serve as members. Chaired by an advanced practice nurse (clinical nurse specialist) and nurse director, the PIT is the group within the organization charged with driving pain practice, education, and quality and research initiatives.
The protocol was then approved via a hierarchical process as follows: (1) nurse practice council; (2) pharmacy and therapeutics committee; (3) medical executive committee; (4) university internal review board; and (5) clinical outcomes committee. Two protocol presentations during separate months were necessary for the pharmacy and therapeutics committee. These entailed initial approval followed by confirmation of required revisions. Two full board reviews by the University of Pittsburgh Internal Review Board were required before this work was deemed a quality assurance project or clinical outcomes study.
Groundwork for protocol implementation
Prior to implementation, IV team nurses, pharmacists and an advanced practice nurse educated care providers throughout the organization about the protocol. Unit-based nurse education included details pertaining to the analgesic, the protocol and the policy. Nurses were taught how to enter a protocol order via a computerized provider order entry system. This was a huge culture change for nurses accustomed to obtaining a written or verbal physician order prior to administering a medication. Supplemental education was included in department specific newsletters such as a critical care newsletter and Needle News, a nurse IV team publication. Pain Resource Nurses were encouraged to role model preemptive analgesia practices among their peers. The protocol or clinical effectiveness guideline is posted on the hospitals intranet along with an L.M.X.4® patient care policy. Both are available for use by all nurses, not just the nurse IV team.
Resident physicians learned about the protocol during regularly occurring educational lunch meetings. It was explained why they should anticipate an increased number of L.M.X.4® protocol orders in their electronic inbox. Pharmacists were taught similarly to nurses. Protocol awareness initiatives included a poster and scholarly presentation at two local nursing research conferences. The poster was displayed within the organization as part of National Nurse Week festivities and showcased as a patient care quality achievement during a state trauma site survey.
The pharmacy department made L.M.X.4® easier to access. Nurse and physician stakeholders on each unit collaborated to decide what medications would be stored in their respective automated drug dispensing systems. Not all patient care units stock the same medications. Topical analgesics were traditionally ordered and then delivered to patient care areas by the pharmacy via a pneumatic tube system. Storing medication in totable IV baskets is not in accordance with national patient safety regulations. In anticipation of these potential hindrances, the pharmacy department made L.M.X.4® uniformly available to all patient care units via an automated drug dispensing system, an endeavor which took several weeks to complete. This provided for protocol order entry with immediate analgesic procurement by nurses.
Data collection
L.M.X.4® usage data are collected from the nurse IV teams electronic spreadsheet-style database. IV team nurses enter the information (self-report). The database includes patient information (i.e. unit, medical record number, visit number, age). The database also includes: (1) procedure; (2) total procedure time; (3) name of the nurse performing the procedure; (4) procedure site; (5) catheter size, if applicable; (6) number of procedure attempts; and (7) topical analgesic use. The IV team supervisor and advanced practice nurse tabulate L.M.X.4® use and report it to the IV team nurses every month.
Conquering barriers
When it became apparent that protocol adherence was slow to occur, the IV team supervisor and an advanced practice nurse led focus groups with the IV team nurses in order to identify barriers. Several care coordination challenges were revealed. During the early protocol implementation phase, the nurse IV team was staffed with 6.5 full-time equivalents (FTEs). Between 5 and 13 nurses filled these FTEs. Staffing fluctuated on a monthly basis for the first several months and more services were being offered with fewer nurses. The new IV team did not inherit the L.M.X.4® protocol; applying the analgesic and waiting for it to take effect was counter to the teams established work flow. Coordinating procedure site selection with acute care non-IV team nurses added extra steps and time. A blitz or competition was started on the acute care floors in an effort to increase L.M.X.4® use and improve care coordination between acute care and IV team nurses. Acute care nurses logged L.M.X.4® doses and high-use units were positively recognized by management.
Barriers related to education and awareness were identified. In-servicing was difficult to accomplish during periods when patient census and acuity were high. Frequent education was offered, even if it was only for one nurse. Laminated posters were hung in medication and treatment rooms and taped to IV baskets to remind the nurses to use L.M.X.4®. Data trends revealed the IV team nurses who implemented the protocol most often. These nurses were positively reinforced and showcased among their peers. In rare instances, nurses applied L.M.X.4® and forgot to document use in the database. Misconceptions about child development, childrens response to pain and anxiety and the benefits of analgesia across the age spectrum were discussed and corrected during IV team staff meetings. The importance of pain reassessment post-analgesic administration and post-procedure was also emphasized and the team was reminded that these are hospital-wide process improvement indicators in accordance with pain standards put forth by the Joint Commission (formerly the Joint Commission on Accreditation of Healthcare Organizations).
Even after a uniform L.M.X.4® supply was accomplished, some nurses maintained it was not available in all patient care areas. This prompted consideration of how the analgesic appeared on the automatic dispensing system screen. Investigators speculated that nurses might not be able to locate the analgesic within the system. L.M.X.4® is listed as the seventh lidocaine preparation entry on the screen menu; a Pain Resource Nurse described this and the need to scroll down to the bottom of the list in a staff newsletter.
Conclusion and future directions
The first nurse-driven analgesic protocol at this organization is a practical application of what pain experts recommend. While nurses are responsible for and hold the key to improved pain control, it is not simple to change historic pain practice. Approval processes can be arduous, even daunting. Protocol implementation did not occur for a full year following submission to the Pain Innovation Team. Nurses who advance such protocols are subject to monthly meeting schedules, characteristic of how most hospital committees operate. Excess scrutiny was given to this protocol because it was the first of its kind and it involved increased independence with medication administration by nurses.
Topical analgesic use by the nurse IV team has increased since the 2005-06 rate of 3 to 4%, but there is room for improvement (see Figure 1). Vigilant reinforcement, barrier elimination and outcome measurement is critical to the success of a nurse-driven pain protocol. Nurses who are strong pain advocates and who demonstrate clinical autonomy must act as role models for their peers and be rewarded (Kramer & Schmalenberg, 2003). The pain knowledge base from which nurses practice must be understood and not assumed. Processes must be aligned to support protocol implementation; this is most efficiently accomplished through interdisciplinary collaboration. A nursing protocol without outcome measurement is meaningless for patients and for an organization. In this case, monitoring practice and data reporting ensures accountability to patients and families, hospital approval bodies and pain management stakeholders.
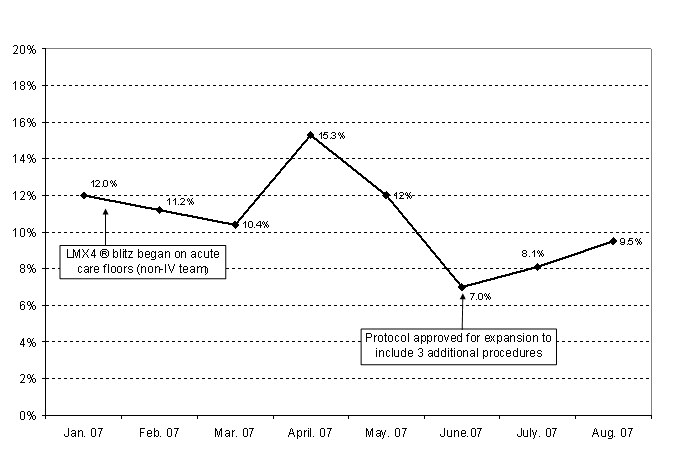
Figure 1. L.M.X.4® usage rate in 2007 for venipuncture and intravenous cannulation procedures by month, Children's Hospital of Pittsburgh Nurse IV Team.
A university-affiliated pediatric level I trauma center provides care for a high acuity patient population. Urgent situations will preclude the use of a topical analgesic for blood work and obtaining line access. Emergency and critical care nurses should consider adapting quality initiatives targeted at improved topical analgesic use (e.g. application at triage) for anticipated procedures.
Currently, the nurse IV team does not document when older patients refuse L.M.X.4®. In general, the median age for application is 4 years, but without patient refusal data this is only a gauge. It appears there is at least an opportunity for improved pain management for the very young child undergoing protocol-specific procedures. Correlation with L.M.X.4® use and the number of procedure attempts and success rates will be helpful in the future and, if compelling, may serve to reinforce protocol adherence. Other disciplines have not objected to using a topical analgesic for the procedures in this study. Furthermore, no protocol-specific adverse drug reactions have been reported.
A venipuncture or intravenous cannulation procedure is considered to be a one nurse IV team service at this hospital. Using L.M.X.4® prior to each is documented as two services. Preemptive analgesia should be inherent in painful procedures. The fact that they are viewed as separate or that pain management is treated as additional may be rooted in pain culture.
This paper is limited only to a report of a protocols effect on nurses use of L.M.X.4®. Despite struggles with achieving higher usage, nurses recent request for protocol expansion to include three additional procedures has been approved, this time taking only two months. The procedures include totally implantable central venous port access, subcutaneous catheter insertion and percutaneous inserted central catheter (PICC) placement. The knowledge-practice gap is closing.
Acknowledgment
The authors extend warm appreciation to Ralph P. DeStefano, Senior Institutional Sales Consultant, Ferndale Laboratories, Inc. and sincere gratitude to Janet O. Aradine, Clinical Effectiveness Specialist.
Tracy Ann Pasek, RN, MSN, CCRN Dawn Thomas, RN Indira Khimji, PharmD Carol Schmitt, PharmD Ann Spence, RN, MS Rebecca Hanni, RN, BSN * All authors are affiliated with Children’s Hospital of Pittsburgh of UPMC, Pittsburgh, Pennsylvania, USA |
References
American Nurses Association. Code of ethics for nurses with interpretive statements, 2001. www.nursingworld.org/MainMenuCategories/ThePracticeofProfessionalNursing/
EthicsStandards/CodeofEthics.aspx
Anand KJ, International Evidence-Based Group for Neonatal Pain. Consensus statement for the prevention and management of pain in the newborn. Arch Pediatr Adolesc Med 2001;155:173-180. PubMed Abstract
Evans NJ, Rutter N. Development of the epidermis in the newborn. Biol Neonate 1986;49:74-80. PubMed Abstract
Flynn AV, Sinclair M. Exploring the relationship between nursing protocols and nursing practice in an Irish intensive care unit. Int J Nurs Pract 2005;11:142-149. PubMed Abstract
Kennedy RM, Luhmann JD. The “ouchless emergency department”. Getting closer: advances in decreasing distress during painful procedures in the emergency department. Pediatr Clin North Am 1999;46:1215-1247. PubMed Abstract
Kramer M, Schmalenberg CE. Magnet hospital staff nurses describe clinical autonomy. Nurs Outlook 2003;51:13-19. PubMed Abstract
Lehr VT, Cepeda E, Frattarelli DAC, Thomas R, LaMothe J, Aranda JV. Lidocaine 4% cream compared with lidocaine 2.5% and prilocaine 2.5% or dorsal penile block for circumcision. Am J Perinatol 2005;22:231-237. PubMed Abstract
MacLean S, Obispo J, Young, KD. The gap between pediatric emergency department procedural pain management treatments available and actual practice. Pediatr Emerg Care, 2007;23:87-93. PubMed Abstract
Meunier-Sham J, Ryan K. Reducing pediatric pain during ED procedures with a nurse-driven protocol: an urban pediatric emergency department’s experience. J Emerg Nurs 2003;29:127-132.
Pitetti RD. Commentary, Do no harm--but first, do not hurt. CMAJ 2005;172:1699.
Taddio A, Shah V, Gilbert-MacLeod C, Katz J. Conditioning and hyperalgesia in newborns exposed to repeated heel lances. JAMA 2002;288:857-861. PubMed Abstract
Taddio A, Soin HK, Schuh S, Koren G, Scolnik D. Liposomal lidocaine to improve procedural success rates and reduce procedural pain among children: a randomized controlled trial. CMAJ 2005;172:1691-1695. PubMed Abstract
Zempsky WT, Cravero JP, American Academy of Pediatrics Committee on Pediatric Emergency Medicine and Section on Anesthesiology and Pain Medicine. Relief of pain and anxiety in pediatric patients in emergency medical systems. Pediatrics, 2004;114:1348-1356. PubMed Abstract