| :: Home :: Editor:
ISSN 1715-3956 |
|
Disclaimer: |
Vol. 16 No. 1-2 |
June 2014 |
Commentary
Pediatric pain psychology fellowship training:
Current trends in the USA and future goals
Rashmi Bhandari, Grace Kao, and Deirdre E. Logan
Action Editor for this manuscript was Carl L. von Baeyer
There is strong evidence supporting the role of psychologists and psychological interventions in pain management. Results from meta-analyses and systematic reviews (Hermann et al., 1995; Eccleston et al., 2002; Trautmann et al., 2006; Eccleston et al., 2009; Palermo et al., 2010; Palermo, 2012) demonstrate that psychological therapies, such as cognitive behavioral therapy interventions, coping strategies, relaxation skills to enhance physiological and emotion regulation (biofeedback and medical hypnosis), patient and family education, and counseling, are effective in reducing pain in children. The strong evidence base underlying these treatment approaches supports the continued specialized training of pediatric pain psychologists.
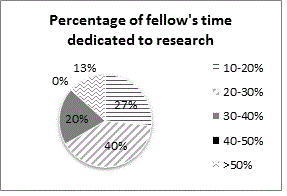
There are currently no standardized requirements or widely adopted curricula in the training of pediatric pain psychologists (Law et al., 2012) in the United States. Although some training programs offer experiences in pain management as part of clinical training in doctoral programs or predoctoral internship, postgraduate fellowship is usually the first opportunity to specialize as a pain psychologist. The aim of the present commentary is to explore steps toward examining and integrating existing curricula and current training approaches of various programs in the USA to aid in efforts to formalize and standardize the training of pediatric pain psychologists. The focus of the current commentary was placed primarily on clinical versus research-based training.
A study of existing pediatric pain curricula was conducted to understand the main components currently emphasized in training. The International Association for the Study of Pain (www.iasp-pain.org) and Pain in Child Health (www.paininchildhealth.dal.ca) are the leading organizations that provide the foundation of knowledge base that can form the framework for the development of formalized training curricula for psychologists specializing in pediatric pain medicine.
International Association for the Study of Pain (IASP) psychology curriculum
The IASP curriculum, first developed in 1995 and regularly updated (most recent revisions in May 2012), provides a framework for the training of psychologists treating pain in general (not specific to the treatment of pain in children). The curriculum aims to: (a) prepare psychologists for pain management knowledge dissemination, (b) introduce and implement techniques and strategies for clinical assessment and intervention, with an emphasis on evidence-based psychological therapies, and (c) understand the impact of psychological factors in pain modulation. Substantial knowledge of pain and implications for assessment and management, including clinical familiarity and/or training is emphasized. Specifically, the curriculum content outline is broken into four main sections: (1) the multidimensional nature of pain, (2) pain assessment and measurement (3) management of pain, and (4) pain syndromes.
Pain in Child Health (PICH) curriculum
PICH is a training initiative sponsored by the Canadian Institutes of Health Research to strengthen the education of individuals (from all disciplines) interested in becoming independent research investigators in pediatric pain medicine. Canadian trainees as well as international trainees (including those from the USA) participate in the training collaborative, which was established in 2002 and is currently funded through 2015. PICH curriculum covers multiple domains of learning, with biological bases, assessment, intervention and prevention, and research serving as key components. Other areas covered include external influences, classification, pharmacology, ethics, and career development. Specific domain content examples reveal a progression of learning from pain knowledge and systems (e.g. physiology, culture, and diseases) to available pharmacological and psychological interventions (e.g. psychological, medications, nerve blocks, complementary and alternative methods) to research and professional development (e.g. work-life balance, managing mental health).
Overall, these curricula are comprehensive, focus on multidisciplinary approaches to pain management and aim to supplement graduate education and training with pain-specific academic, professional knowledge and clinical experience. From these models, guidelines may be drawn for tailoring the postdoctoral training of psychologists who want to specialize in pediatric pain medicine. However, to date in the United States, the education, application and delivery, practice and experience of postdoctoral trainees are largely left to the discretion of individual programs and training directors.
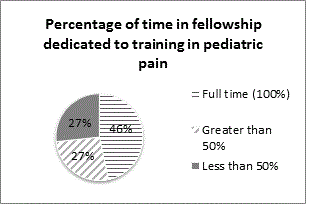
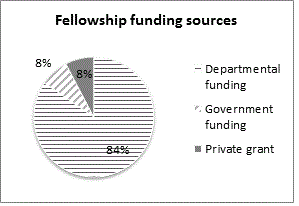
To understand the current state of pediatric pain psychology training in the USA, a broad evaluation and needs assessment was begun through an exploratory survey process. A brief questionnaire of 10 items was constructed by the authors to survey members of the American Psychological Association’s Society of Pediatric Psychology (APA Division 54) via their email list and was disseminated in September 2013. The email list includes psychologists with interests spanning all of pediatric psychology and is not specific to those focusing on pain management, but it was judged to be the best venue for reaching relevant training faculty in the USA. Fourteen training directors responded to this survey (American Pain Society [APS] lists 34 American-based pediatric pain programs although it is unclear how many of those programs offer pain psychology training). Of responses received, seven programs dedicated 100% of their training to pain. The majority (84%) of the fellowships were funded by departmental funds. Please see the appendix for details of programs.
The format of most postdoctoral pediatric pain psychology fellowships in the USA consists of a single fellow, under supervision of one to two faculty members, developing competencies based on clinical interactions with patients with acute, recurrent, palliative and chronic complex pain syndromes, most commonly in a 12-month training position. Most programs provide training via participation in clinical settings (combination of outpatient, inpatient and rehabilitation assessment and treatment) with supervision and didactics. Two programs fund formal training in biofeedback, and one program in self-hypnosis. Advantages to this structure are opportunities for close supervision, focused and individualized person-centered training, and flexibility to tailor experiences according to the fellow’s professional goals and needs. Excellence in patient-centered treatment requires that clinicians respond to patients in a compassionate and knowledgeable fashion, giving rise to the need to add curricular content. Half of the programs that participated reported the use of a formal curriculum. Geographic and communication barriers present the major challenges to standardization of curriculum and collaboration across training programs. As the state of training for future pediatric pain psychologists is reviewed, the development of a standardized collaborative curriculum emerges as a core need.
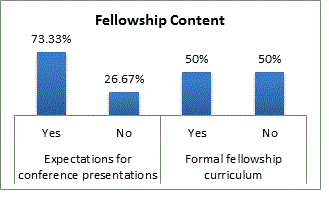
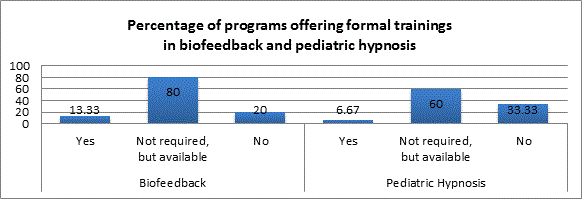
Additionally, most program directors reported the desire to participate in cross-site training and collaborative research, develop shared curriculum guidelines, create opportunities for networking and support for fellows, incorporate formalized training, and share didactics (webinars). Greater, more formalized organization among training directors may help desires for increased collaboration across training sites be realized. In fact, recent efforts toward this goal have led to the establishment of a monthly, multi-site conference call where fellows from pediatric pain programs across the USA have the opportunity to build their networks, receive/give support, and set the stage for shared learning.
Future improvements in pediatric pain psychology training in the USA should include efforts to develop a collaborative training network. Relevant national organizations such as APA Division 54 and APS, and international organizations such as IASP (special interest group on pain in childhood) and PICH, may be sources to tap to provide structure and logistical support for such efforts (e.g. small training-focused grants for the establishment of a taskforce to provide guidance in the relevant education components, length of fellowship, prerequisite program). In Canada, the PICH initiative has benefited both from government and foundation grant support, along with dedicated faculty leadership and an administrative structure. Similar support from the US government, foundations, and academic institutions could enhance opportunities for trainees. If successful, the existence of such a network would benefit not only trainee education but also clinical care and research missions in the treatment of pediatric pain. In conclusion we suggest the following next steps toward accomplishing the important goal of strengthening the education and development of emerging pediatric pain psychologists in the USA:
-
Provide formal training in evidence-based psychological treatments for pediatric pain such as self-hypnosis and biofeedback (Tsao & Zeltzer, 2005) and cognitive-behavior therapy for pain in children (Eccleston et al., 2002; Palermo, 2012).
-
Provide formal training to enhance ability to function within a multidisciplinary team and sharpen the following skills:
-
Communicate biopsychosocial and non-dualistic model of pain symptoms to patients, families, and other professionals.
-
Understand the role of physical therapy and reconditioning in the process of rehabilitation or health maintenance (desensitization, transcutaneous electrical nerve stimulation [TENS], etc.).
-
Know basic pharmacology (benefits, side effects) and pharmacokinetics of analgesics.
-
Understand the role of complementary and alternative therapy for pain management (acupuncture, hypnosis, biofeedback, music therapy, art therapy, etc.).
-
Be aware of functional, educational, and vocational rehabilitation (formal and informal accommodations, need for special education services, etc.).
-
Understand the concept of hospice and palliative care.
-
Continue to develop the emerging collaborative network of training supervisors/directors of pediatric psychology training programs. Work toward the development of best practice guidelines regarding structure of fellowship training, length of fellowship, key learning objectives and experiences.
-
Continue to pilot multisite training initiatives using both technology assistance (e.g. virtual seminars) and in-person training workshops organized around key national conferences. Obtain feedback from participants to assess value of these experiences and areas for expanded collaborative training opportunities. Examples of training workshops could include: the most commonly used nerve blocks and pharmacology for pain management in children, modules on the most common pediatric pain syndromes, somatoform disorders.
-
Enlist leadership in pediatric interest groups of the APS, IASP and the pain special interest group of APA Division 54 to organize subcommittees focused on education goals, both interdisciplinary and discipline-specific. IASP may be particularly helpful in aligning any US-specific efforts with international efforts.
-
Identify potential funding sources to support and expand these educational efforts.
Rashmi Bhandari, PhD Grace Kao, PhD Deirdre E. Logan, PhD |
Cite as: Bhandari R, Kao G, Logan DE. Pediatric pain psychology fellowship training: Current trends in the USA and future goals. Pediatric Pain Letter 2014;16(1-2):22-28. www.childpain.org/ppl
Appendix
Pediatric pain psychology postdoctoral training programs listed alphabetically by state
Program |
Location |
Number and duration of positions |
Training director(s) |
Brief Description |
University of Southern California-University of Southern California Center for Excellence in Developmental Disabilities and Children’s Hospital Los Angeles Keck School of Medicine |
California |
2 fellows/ year 2 year position |
Sara Sherer, PhD Jeffrey I. Gold, PhD |
Postdoctoral fellowship with training offered in pediatric pain management. |
Pediatric Pain Management Clinic, Lucile Salter Packard Children’s Hospital/ Stanford University Medical Center |
California |
1 fellow/ year 1 year position |
Rashmi Bhandari, PhD |
Postdoctoral fellowship in pediatric pain psychology with training offered in outpatient, intensive rehabilitation, and inpatient settings, as well as research opportunities in pediatric pain. |
Children’s National Medical Center |
District of Columbia |
1 fellow/ year 1 year position |
Angela Fletcher, PsyD |
Postdoctoral fellowship in the Department of Behavioral Pain Medicine with multidisciplinary model incorporating trainees at multiple levels of training. Services provided include outpatient therapy and inpatient consultation/liaison. |
Kennedy Krieger Institute |
Maryland |
1 fellow/ year 1 year position |
Cynthia Ward, PsyD |
Postdoctoral fellowship in the Pediatric Psychology Consultation Program that conducts evaluation and provides treatment for pain management outpatient and inpatient rehabilitation, as well as general consultation/liaison services. |
Boston Children’s Hospital Pain Treatment Service |
Massachusetts |
1 fellow/ year 1-2 year position |
Deirdre Logan, PhD |
Postdoctoral fellowship in pediatric pain psychology with training offerings in outpatient and intensive rehabilitation, as well as research opportunities in pediatric pain. |
Mayo Clinic |
Minnesota |
1-2 positions/ year, not all positions pain-focused 2 year fellowship |
Cynthia Harbeck-Weber, PhD ABPP |
Clinical child fellowship with clinical and research training experiences in the pain outpatient clinic, intensive pain rehabilitation, and consultation liaison programs. |
Cleveland Clinic Children’s Hospital |
Ohio |
Contact for details. |
Ethan Bemore, PhD |
Postdoctoral fellowship training program is expected to begin September 2014. |
Nationwide Children’s Hospital |
Ohio |
1 fellow/ year 1 year position |
Kathleen Lemanek, PhD |
Postdoctoral psychology fellowship with training offered in interdisciplinary clinics and consultation-liaison service. |
University of Oklahoma Health Sciences Center |
Oklahoma |
Contact for details. |
Stephen Gillaspy, PhD |
Postdoctoral fellowship in pediatric psychology with training offered in pain management in various clinics. |
Oregon Health and Science University Child Development and Rehabilitation Center |
Oregon |
1 fellow/ year 1-2 year position |
Anna Wilson, PhD Kurt Freeman, PhD |
Postdoctoral psychology fellowship with training offered in pediatric pain management. Includes outpatient assessment and treatment as part of interdisciplinary pain management clinic, as well as inpatient pain consultation and involvement in pain research activities. |
St. Jude Children’s Research Hospital |
Tennessee |
4 fellows/ year 2 year fellowship with 6 months training in pain |
Valerie Crabtree, PhD Jennifer Ehrentraut, PhD |
Postdoctoral psychology fellowship with training offered in pediatric pain management. |
Seattle Children’s Hospital Research Institute, Palermo Lab |
Washington |
4 fellows/ year 1-2 year position |
Tonya Palermo, PhD |
Psychology postdoctoral fellowship in pediatric pain research with opportunities for involvement in clinically focused (intervention) research. Opportunities also exist for clinical activities with the Pain Clinic at Seattle Children’s Hospital. |
Chronic Pain and Headache Clinics at Children’s Hospital of Wisconsin |
Wisconsin |
1 fellow/ year 1 year position |
Kim Anderson Khan, PsyD |
Postdoctoral psychology fellowship with training offered in outpatient pediatric pain management as well as research opportunities in pediatric pain. |
References
Eccleston C, Morley S, Williams A, Yorke L, Mastroyannopoulou K. Systematic review of randomised controlled trials of psychological therapy for chronic pain in children and adolescents, with a subset meta-analysis of pain relief. Pain 2002;99:157-165. PubMed Abstract
Eccleston C, Palermo TM, Williams AC, Lewandowski A, Morley S. Psychological therapies for the management of chronic and recurrent pain in children and adolescents. Cochrane Database Syst Rev 2009 Apr 15;(2):CD003968. PubMed Abstract
Hermann C, Kim M, Blanchard EB. Behavioral and prophylactic pharmacological intervention studies of pediatric migraine: an exploratory meta-analysis. Pain 1995;60:239-255. PubMed Abstract
Law EF, Palermo TM, Walco GA. The making of a pediatric pain psychologist: education, training, and career trajectories. Pain Manag 2012;2:499-507. PubMed Abstract
Palermo TM. Cognitive-behavioral therapy for chronic pain in children and adolescents. New York: Oxford University Press, 2012. Link
Palermo TM, Eccleston C, Lewandowski AS, Williams AC, Morley S. Randomized controlled trials of psychological therapies for management of chronic pain in children and adolescents: an updated meta-analytic review. Pain 2010;148:387-397. PubMed Abstract
Trautmann E, Lackschewitz H, Kröner-Herwig B. Psychological treatment of recurrent headache in children and adolescents - a meta-analysis. Cephalalgia 2006;26:1411-1426. PubMed Abstract
Tsao JC, Zeltzer LK. Complementary and alternative medicine approaches for pediatric pain: a review of the state of the science. Evid Based Complement Alternat Med 2005;2:149-159. PubMed Abstract

