| :: Home :: Editor: ISSN 1715-3956 |
|
Disclaimer: |
Vol. 11 No. 2 |
August 2009 |
Commentary
Iyengar yoga for pediatric chronic pain
Subhadra Evans, Jennie Tsao and Lonnie Zeltzer
Yoga is a discipline developed in ancient India, characterized as a science of self-study and awareness through asanas (body postures), pranayama (patterns of breathing), and meditation. Yoga has been embraced in Western settings as a form of exercise and relaxation. Currently, yoga programs are relatively low cost, widely available, and safe when performed properly. Despite the wide use of yoga in the community, little research exists to demonstrate the safety and efficacy of yoga to address health problems and to promote well-being in children. In the Pediatric Pain Program at UCLA we are currently attempting to address this gap in the literature by conducting a series of yoga interventions for young people with chronic pain. In this commentary, we will introduce the reader to Iyengar yoga (IY), provide a summary of our work in the area including the development of a theoretical model, and outline future research directions.
IY is distinct from other traditions of yoga in its emphasis on anatomical alignment, use of props, sequences of postures that are tailored for medical conditions, and systematized teacher training that includes knowledge of physiology, anatomy and yoga philosophy (Iyengar, 2008). Teachers study for at least 7 years before being certified to work with students who have therapeutic needs, including children with chronic pain. Training includes the modification of poses for individuals with physical limitations and the use of props to prevent straining and injuries. Given their training in the use of yoga for people with physical limitations, IY teachers certified in therapeutics may be considered suitable for chronic pain patients. Not all styles of yoga demonstrate an extensive teacher training system and caution must be exercised in recommending yoga classes that do not have a demonstrable teacher training program or experience with medical populations.
Pediatric yoga research
Only one study has been published examining yoga for chronic pain in children. In this study, 25 patients with irritable bowel syndrome (IBS) aged 11-18 years (mean 14.15 years) were randomized to a 4-week home-practice of yoga, subsequent to an initial training session or to a waitlist control condition (Kuttner et al., 2006). The instructor was certified in Hatha and Iyengar yoga, although it is unclear which yoga tradition was used in the instructional session and video. A number of standardized questionnaires related to IBS symptoms and psychological functioning were examined. Adolescents in the yoga group exhibited trends towards improved disability, coping, and anxiety following yoga relative to adolescents in the waitlist condition. There were no differences on pain, depression or overall gastrointestinal symptoms. Importantly, adolescents reported that the intervention was helpful, and the authors provided a detailed summary of the yoga poses used. However, it is unclear to what degree participants practiced yoga and to what extent they adhered to the prescribed yoga protocol.
One of the most significant criticisms facing the research on yoga to date has been a lack of transparency regarding the tradition of yoga utilized, including information regarding poses, teacher training, teacher adherence to the intervention and presence of adverse events (Evans et al., 2008). There is great variation across the numerous schools of yoga and a lack of standardization can confound interpretations of the overall efficacy of yoga on illness states.
In order to empirically test the safety, feasibility and efficacy of IY for young people, we recently conducted a pilot study for patients with rheumatoid arthritis (RA). The study involved a single-arm group-administered 6-week biweekly Iyengar yoga (IY) program for 8 young adults aged 24-31 years of age with RA. Treatment outcomes were evaluated using a mixed-methods approach that combined quantitative results from standardized questionnaires (including the SF-36, Functional Disability Inventory, BSI-18 and numeric rating scales) and qualitative interviews with participants. Initial attrition was 37% (n = 3) after the first week due to scheduling conflicts and a prior non-RA related injury. However, the remaining participants (n = 5) completed 75-100% of treatment sessions (M = 95%). No adverse events were reported. The quantitative results indicated significant improvements in pain, pain disability, depression, mental health, vitality and self-efficacy. Interview data demonstrated a high degree of cross-validation with quantitative data although some participants expressed uncertainty regarding the impact of IY on their arthritis-specific pain. Nevertheless, participants consistently reported that yoga helped with their energy, relaxation and mood and they also revealed perceived mechanisms for how yoga impacted well-being, including physical changes (e.g. range of motion, physiological awareness), and psychospiritual developments (e.g. acceptance, coping, self-efficacy, mindfulness). These preliminary findings indicate that IY may be a safe, feasible and effective complementary approach for young people with RA.
Yoga in the clinic
We recently conducted a survey of treatment expectations and patient preferences for complementary and alternative medicine (CAM) among children with chronic pain and their families (Tsao et al., 2005; Tsao et al., 2007). Participants were 129 children and adolescents (94 girls; age 8 to 18 years, M = 14.5 years) presenting to our pain clinic. Notably, we found that yoga was among the top three most popular CAM interventions. These findings suggest that yoga is an attractive treatment approach for young people with chronic illness who are interested in CAM. IY has been offered for many years as part of the clinical treatment package offered at UCLA. Anecdotally, we have found that children and adolescents dealing with a range of chronic pain conditions experience a reduction in symptoms following IY.
Anecdotal evidence in the clinic points to the utility of using IY therapeutically especially for conditions which may benefit from psychological and physical treatment, such as juvenile idiopathic arthritis (JIA). Recently, a 15-year-old female diagnosed 4 years previously with JIA presented to the clinic with intractable headaches and periodic flares of arthritis that caused her distress and often kept her from school. She began working with an IY teacher doing a series of poses established for headache and arthritis. The patient gradually became stronger and had less pain. As her competency with the group of yoga poses increased, the patient’s analgesic medication usage decreased and she reported feeling more in control of her body. These benefits are common to patients who choose IY as part of their pain management plan in our program. Thus far, there have been no adverse events from yoga in our clinic or research populations and the risks appear minimal with a sufficiently trained and certified IY teacher.
A model to account for benefits
Chronic pain is best understood from a biopsychosocial perspective: psychological, biological, and social factors are understood to interact in the etiology and maintenance of pain (Gatchel et al., 2007). This model can also be used to guide the conceptual understanding of how yoga may improve functioning in patients. The model depicted below is based on our recently published work (Evans et al., 2009). Derived from the biopsychosocial model of pain and the yoga literature, Figure 1 depicts a conceptual model of how IY may improve pain and functioning.
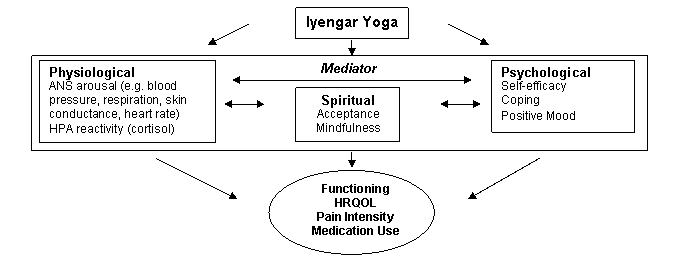
Figure 1. Conceptual model of Iyengar Yoga for chronic pain. Note. ANS: Autonomic Nervous System; HPA: Hypothalamic-Pituitary-Adrenal Axis; HRQOL: Health-Related Quality of Life.
Physiological mechanisms. It is thought that yoga quiets the body as well as the mind through attention, and vascular and muscular relaxation (Monro et al., 1995). Yoga has been associated with a number of physiological benefits. Research linking yoga with autonomic nervous system functioning has found improved physiologic responses, including reduced diastolic and systolic blood pressure, decreased heart rate, and increased heart rate variability, indicative of healthy functioning (Bharshankar et al., 2003; McCaffrey et al., 2005; Sivasankaran et al., 2006; Khattab et al., 2007). Iyengar yoga appears to be especially involved in enhancement of cardiac parasympathetic system modulation, consistent with a reduction in stress response pathophysiology (Khattab et al., 2007).
Psychological mechanisms. Yoga has a number of positive effects on psychological functioning that have been reported in healthy, pain, and stress groups and for a wide variety of age groups. Two recent reviews examining yoga as a treatment for individuals with depression and anxiety underscored the promise of yoga for elevating mood. Out of 5 randomized controlled trials (RCT) examining the use of yoga for individuals with depression, beneficial effects were reported in 4 (Kirkwood et al., 2005). All 8 randomized studies of yoga used for individuals with clinical anxiety disorders reported a reduction in symptoms following yoga (Pilkington et al., 2005). For example, Woolery et al. (2004) reported reduced depression and anxiety after a 5-week IY program in young adults with depression. Other positive psychological effects include coping and self-efficacy (Kuttner et al., 2006). Persisting in a yoga class promotes a sense of accomplishment that is consistent with the development of self-efficacy. Self-efficacy, effective coping, and positive psychological functioning, in turn, are related to better physical functioning in patients experiencing chronic pain and illness (Schanberg et al., 1997).
Spiritual processes. Related to the psychological benefits of yoga are mindfulness and acceptance. Although these skills have been incorporated into mainstream psychology, their roots can be traced to Eastern spiritual practices. Yoga is associated with a mastery of life challenges, which may extend to dealing with pain (Raub, 2002). As noted by Iyengar, “The pain is there as a teacher…We must try not to run from pain but to move through it and beyond it” (2005, p. 47). Yoga may enhance patients’ acceptance of health, which involves noting the pain without avoidance or limited participation in life goals (McCracken & Vowles, 2008). Such acceptance appears to be particularly important in coping with chronic conditions (Mason et al., 2008). IY is also associated with mindful awareness, or an openness to present moment experiences. Mindful activity has been found to improve mood and stress (Netz & Lidor, 2003) likely through strengthening attention on the present (Monro et al., 1995). Use and control of attention can be turned towards minimizing stress, disability and pain. In our recent pilot study, patients reported enhanced mindfulness in a number of ways such as by being more aware of stress, alignment and letting go of pain.
Future directions
Presently we are conducting additional yoga studies, including an RCT of IY for pediatric patients with IBS, with the intention to further explore potential biopsychosocial mechanisms in the impact of yoga upon children’s functioning. These and further studies are needed to assess the efficacy of yoga using rigorous methodology including standardized measures of treatment outcome and manualized protocols in clinical child populations. Long-term research is needed to determine whether yoga has a general beneficial effect on patients, or whether there are certain conditions that represent a good match with yoga. A number of challenges and barriers to treatment are likely to exist, which must also be explored. As with most behavioral interventions with children, the support of parents is paramount. It is not known to what extent parents will accommodate their child’s participation which may require parents to drive their child long distances two or more times per week. Another issue is the development of child-validated questionnaires to assess mechanisms of action, including a validated mindfulness measure for children. It appears that IY offers a promising adjunct treatment in the clinical care of young patients with chronic pain, although research in this area must begin in earnest before making definitive recommendations.
Subhadra Evans, PhD Jennie Tsao, PhD Lonnie Zeltzer, MD |
References
Bharshankar JR, Bharshankar RN, Deshpande VN, Kaore SB, Gosavi GB. Effect of yoga on cardiovascular system in subjects above 40 years. Indian J Physiol Pharmacol 2003;47:202-206. PubMed Abstract
Evans S, Subramanian S, Sternlieb B. Yoga as treatment for chronic pain conditions: a literature review. Int J Disabil Hum Dev 2008;7:25-32.
Evans S, Tsao JCI, Sternlieb B, Zeltzer LK. Using the biopsychosocial model to understand the health benefits of yoga. J Complement Integr Med 2009;6:Article 15. www.bepress.com/jcim/vol6/iss1/15
Gatchel RJ, Peng YB, Peters ML, Fuchs PN, Turk DC. The biopsychosocial approach to chronic pain: scientific advances and future directions. Psychol Bull 2007;133:581-624. PubMed Abstract
Iyengar BKS. Light on life: the yoga journey to wholeness, inner peace, and ultimate freedom. Emmaus, PA: Rodale, 2005.
Iyengar BKS. Yoga the path to holistic health. London: Dorling Kindersley, 2008.
Khattab K, Khattab AA, Ortak J, Richardt G, Bonnemeier H. Iyengar yoga increases cardiac parasympathetic nervous modulation among healthy yoga practitioners. Evid Based Complement Alternat Med 2007;4:511-517. PubMed Abstract
Kirkwood G, Rampes H, Tuffrey V, Richardson J, Pilkington K. Yoga for anxiety: a systematic review of the research evidence. Br J Sports Med 2005;39:884-891. PubMed Abstract
Kuttner L, Chambers CT, Hardial J, Israel DM, Jacobson K, Evans K. A randomized trial of yoga for adolescents with irritable bowel syndrome. Pain Res Manag 2006;11:217-223. PubMed Abstract
Mason VL, Mathias B, Skevington SM. Accepting low back pain: is it related to a good quality of life? Clin J Pain 2008;24:22-29. PubMed Abstract
McCaffrey R, Ruknui P, Hatthakit U, Kasetsomboon P. The effects of yoga on hypertensive persons in Thailand. Holist Nurs Pract 2005;19:173-180. PubMed Abstract
McCracken LM, Vowles KE. A prospective analysis of acceptance of pain and values-based action in patients with chronic pain. Health Psychol 2008;27:215-220. PubMed Abstract
Monro R, Nagarathna R, Nagendra HR. Yoga for common ailments. New York/London: Simon & Schuster, 1991.
Netz Y, Lidor R. Mood alterations in mindful versus aerobic exercise modes. J Psychol 2003;137:405-419. PubMed Abstract
Pilkington K, Kirkwood G, Rampes H, Richardson J. Yoga for depression: the research evidence. J Affect Disord 2005;89:13-24. PubMed Abstract
Raub JA. Psychophysiologic effects of Hatha Yoga on musculoskeletal and cardiopulmonary function: a literature review. J Altern Complement Med 2002;8:797-812. PubMed Abstract
Schanberg LE, Lefebvre JC, Keefe FJ, Kredich DW, Gil KM. Pain coping and the pain experience in children with juvenile chronic arthritis. Pain 1997;73:181-189. PubMed Abstract
Sivasankaran S, Pollard-Quintner S, Sachdeva R, Pugeda J, Hoq SM, Zarich SW. The effect of a six-week program of yoga and meditation on brachial artery reactivity: do psychosocial interventions affect vascular tone? Clin Cardiol 2006;29:393-398. PubMed Abstract
Tsao JC, Meldrum M, Bursch B, Jacob MC, Kim SC, Zeltzer LK. Treatment expectations for CAM interventions in pediatric chronic pain patients and their parents. Evid Based Complement Alternat Med 2005;2:521-527. PubMed Abstract
Tsao JCI, Meldrum M, Kim SC, Jacob MC, Zeltzer LK. Treatment preferences for CAM in children with chronic pain. Evid Based Complement Alternat Med 2007;4:367-374. PubMed Abstract
Woolery A, Myers H, Sternlieb B, Zeltzer L. A yoga intervention for young adults with elevated symptoms of depression. Altern Ther Health Med 2004;10:60-63. PubMed Abstract

